My Reasoning for Minimally Invasive Shoulder Replacement
Why I adopted a 5 cm mini-incision approach with 3D planning and patient-specific technology — and what it means for your recovery.
Shoulder replacement surgery has evolved considerably in recent years. While the core goals — relieving pain and restoring function — remain unchanged, the way we achieve those goals has advanced significantly.
Since February 2025, I have been performing shoulder joint replacement through a refined minimally invasive technique using a 5 cm incision, combined with 3D pre-operative planning and patient-specific surgical guides. Every case I have undertaken since adopting this approach has been performed this way, including patients with severe deformity requiring augmented reconstructions.
This article explains the reasoning behind my approach and what you, as a patient, can expect.
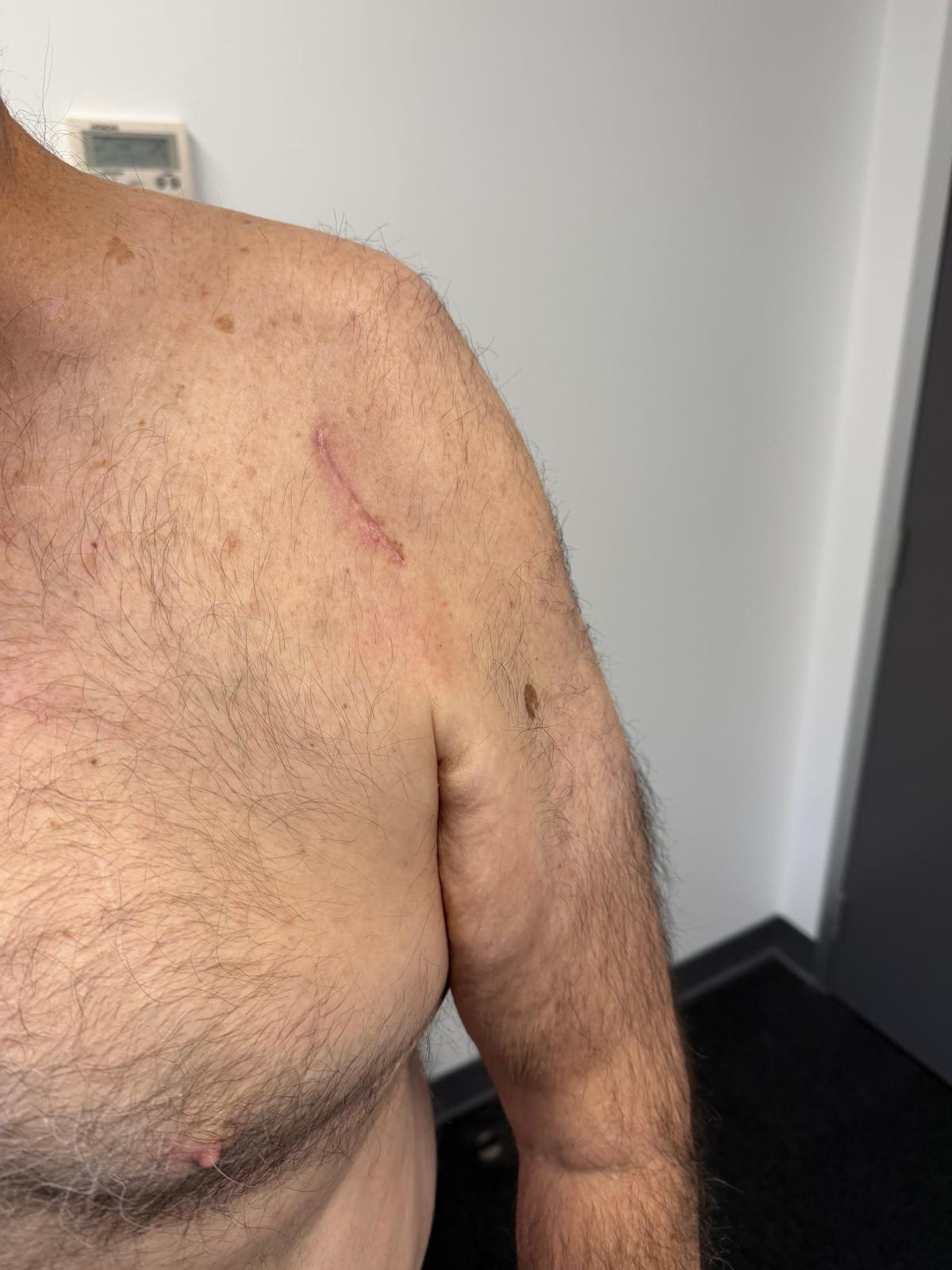
01 — The Mini-Incision Technique
Less Disruption, Faster Recovery
A 5 cm incision changes the recovery equation
Traditional shoulder replacement typically involves incisions of 10 to 15 cm and significant retraction of the surrounding soft tissue. My mini-incision approach uses a 5 cm skin opening — roughly a third of the conventional length. This is not simply a cosmetic difference. A smaller incision means less disruption to the deltoid and surrounding muscles, reduced surgical trauma to soft tissue, and a faster return to normal shoulder mechanics post-operatively.
The deltoid and anterior muscles are gently separated just enough to access the joint — without unnecessary cutting of muscle attachments. Preserving these structures is fundamental to the quality of the patient's recovery.
Less surgical trauma
Reduced postoperative pain
Improved return to function
Faster recovery
Smaller, more discreet scar
Soft-tissue preservation
02 — 3D Planning & Patient-Specific Technology
Precision Before Entering Theatre
Customised surgery, designed weeks in advance
Accurate implant positioning is one of the most important determinants of long-term shoulder replacement success. For every patient I treat, I use 3D CT imaging to perform virtual surgery before you arrive at hospital. This allows me to understand your exact bone geometry — the unique shape and dimensions of your humeral head and glenoid socket — and select the ideal implant size and placement in advance.
From this planning, patient-specific surgical guides are manufactured. These precision tools are matched to your anatomy and used during the procedure to achieve the implant placement we planned digitally. After the components are secured, a post-operative X-ray is taken while you are still in theatre to confirm accurate placement.
03 — Who Can Benefit
Conditions Treated
A thorough assessment guides every decision
I endeavour to use this minimally invasive approach for all patients. Following a comprehensive consultation, physical examination, and review of imaging, I will confirm whether the mini-incision technique is appropriate for your anatomy and condition.
-
Shoulder OsteoarthritisThe most common reason for shoulder replacement. Cartilage wear causes progressive pain, stiffness, and loss of motion — particularly in people over 60.
-
Rheumatoid & Inflammatory ArthritisWhen autoimmune inflammation has destroyed the joint lining and medications are no longer effective, replacement can restore function.
-
Rotator Cuff ArthropathyA long-standing massive rotator cuff tear can lead to secondary arthritis. A reverse shoulder replacement is typically the best solution.
-
Avascular Necrosis (AVN)When blood supply to the humeral head is disrupted and the bone collapses, shoulder replacement relieves pain and restores motion.
-
Complex Proximal Humerus FracturesIn severe fractures — especially where the bone is shattered or blood supply is compromised — replacement offers the best chance at long-term function.
04 — Recovery & Outcomes
What to Expect After Surgery
Your commitment to rehabilitation shapes your outcome
Following surgery, your arm will be supported in a sling for two to four weeks. Early physiotherapy begins shortly after surgery to restore mobility and build strength. Patient commitment to prescribed home exercises has a direct and significant influence on the final result.
Light daily activities — dressing, eating — can typically resume within the first couple of weeks. Driving generally follows several weeks later, once adequate strength and control return. More demanding tasks and overhead lifting usually wait until eight to twelve weeks or beyond, guided by your physiotherapy progress.
When both surgical technique and implant selection are well-matched to the patient, shoulder replacement implants can last fifteen to twenty years or more. Careful follow-up and avoiding excessive joint stress are important for long-term longevity.
Download Approach Overview
A detailed explanation of the minimally invasive technique and 3D planning in total shoulder replacement.
